A multi-centre study of the risk factors and the impact of endometriosis on health-related quality of life: A pilot study
A pilot study (also known as a feasibility study) is a small-scale study designed to test logistics and gather information prior to a larger study, in order to improve the latter’s quality and efficiency (Lancaster 2004). The GSWH pilot study was carried out between the first week of July and 8 August 2008. For the study, eligible women were recruited from the Nuffield Department of Obstetrics and Gynaecology (NDOG) clinics to assess the feasibility of the agreed protocol for the GSWH. We embarked on the GSWH pilot study principally to test the feasibility of the study protocol. The pilot study also presented an opportunity to test the administration of patient and surgical questionnaires, specifically assessing comprehensibility, appropriateness and clarity of definitions in the questions. It also allowed an initial assessment of consistency in the presentation and whether the questions asked could be easily understood. The consent forms and patient information leaflets were also assessed for similar characteristics in the pilot study. Understanding the rate of uptake of invitation in the pilot study provided information that guided planning for the length of recruitment. Reasons for declining an invitation informed approaches to enhancing uptake rate in the main study.
The following sections summarise the method and key outcomes of the pilot study.
In the pilot study, we invited women who were between the ages of 18 and 45 years and who were attending the Nuffield Department of Obstetrics and Gynaecology (NDOG) clinics to participate in the study. We scheduled them for laparoscopy either on account of symptoms for which endometriosis could be a cause or for tubal sterilisation. Eligible women, who did not have a previous surgical diagnosis of endometriosis, were identified by the research assistant on a weekly basis from the operating lists of the department and were sent letters inviting them to participate in the study. This recruitment method had been shown to be most successful in previous studies conducted at NDOG, as it facilitates a comprehensive identification of eligible women and maximum recruitment rates. Consenting women had the option of either completing the online questionnaire or requesting a paper copy from the research assistant.
On each day of scheduled surgery, the research assistant checked the nurse administration database online to establish whether the woman about to undergo surgery had been invited to take part in the study and if she had completed an online questionnaire. If she had done so, her surgical sheet was completed first on paper and then online post-op. If she had consented to take part but had not completed an online questionnaire, the research assistant invited her to complete the paper version before her surgery. If women had not completed the questionnaire before surgery, they were not asked to do so after the operation.
An episode of invitation was considered closed only when an eligible woman had undergone surgery without completing a questionnaire either online or on paper. Therefore, the denominator for response rates is the number of women who were sent invitation letters and had undergone their laparoscopy over the period of the pilot study.
Basic data analysis was carried out after six weeks of recruitment. Response rate was calculated as the proportion of eligible women who agreed to participate. Reasons for non-participation were explored and documented by the research assistant via telephone conversations with those who had declined. The proportion of completed questionnaires entered either directly online or initially on paper, were assessed to give an indication of how participants used either medium of response.
The demographic and other characteristics of the pilot study population were described: age, marital status, education, ethnicity, reasons for investigation, age at menarche, duration of periods in the last three months, cycle length and Body Mass Index (BMI). Although the small sample size limited how much could be inferred from the results, comparisons in some of the above parameters were made between women with and without endometriosis.
The SF-36 questionnaire was also analysed. The questionnaire comprised one transitional question and 35 items divided into eight sections: physical function (ten items), role limitation owing to physical problems (four items), body pain (two items), health perception (five items), vitality (four items), social functioning (two items), role limitation owing to emotional problems (three items) and mental health (five items). For each scale, responses were assigned scores from 0 (worst health state) to 100 (best health state).
For the statistical analysis, data was expressed as medians, 25th percentiles and 75th percentiles. Preliminary, basic descriptive statistics suggested that the distributions for ‘health perception’ and ‘vitality’ were normal in our population but the distributions of other scales were non-normal. However, statistical analyses did not make any assumptions about normality for any of the scales owing to the very small sample size (n=19). The Mann-Whitney U test was used to assess the difference between scores of women with and without endometriosis on each of the scales.
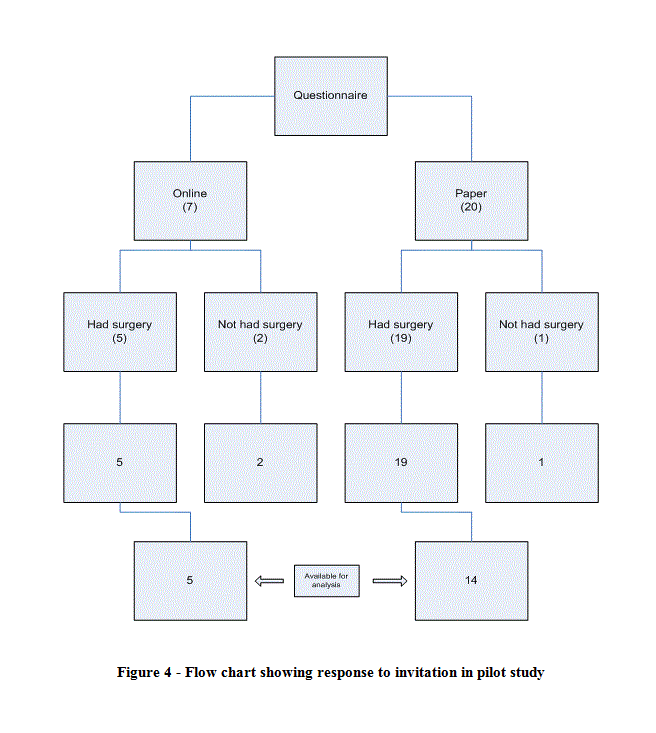
Over the period of the pilot study, 32 invited eligible women underwent laparoscopic surgery. Of these women, 27 took part in the study, yielding a response rate of 84.4%. Of the five women who did not take part, one did not speak any English and the other four gave no specific reasons for their non-participation.
As Figure 1 below shows, only 26% of responses were online, most women having chosen to complete the paper version of the questionnaire. Only records for which there were complete patient and surgical questionnaires were available for analysis. All five online responses eligible for analysis were included in the analysis but only 14 of the 19 eligible paper responses were available for analysis. Of the five that were not available for analysis, two were complete paper questionnaires with no accompanying surgical sheets and three were surgical sheets unaccompanied by questionnaires. The latter were most likely to be the records of women who began completing paper questionnaires on the morning of their surgery but could not finish doing so before they went in for surgery.

As shown in Table 3 above, most of the women who were enrolled in the pilot study were 30 to 34-year-old married women of white ethnicity, most of whom were university-educated. The commonest reasons for laparoscopy were for investigation of pelvic pain and infertility (nearly 60% of the women were infertile). Of the 19 women, nine (47%) were diagnosed with endometriosis at surgery.
Although the very small sample size did not allow meaningful statistical analyses, there were indications that women who underwent laparoscopy on account of pelvic pain had 3.2 greater unadjusted odds of having been diagnosed with endometriosis at laparoscopy than those without pelvic pain (OR=3.2 (95% CI: 0.42 – 24.4). Women who underwent laparoscopy on account of infertility had 1.3 greater unadjusted odds of having been diagnosed with endometriosis at laparoscopy than those not reporting infertility (OR=1.3 (95% CI: 0.20 – 8.71).
The sample size was deemed too small to allow in-depth analysis to examine risk factors for endometriosis.
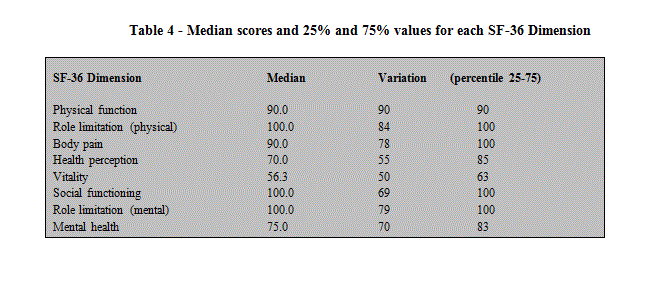
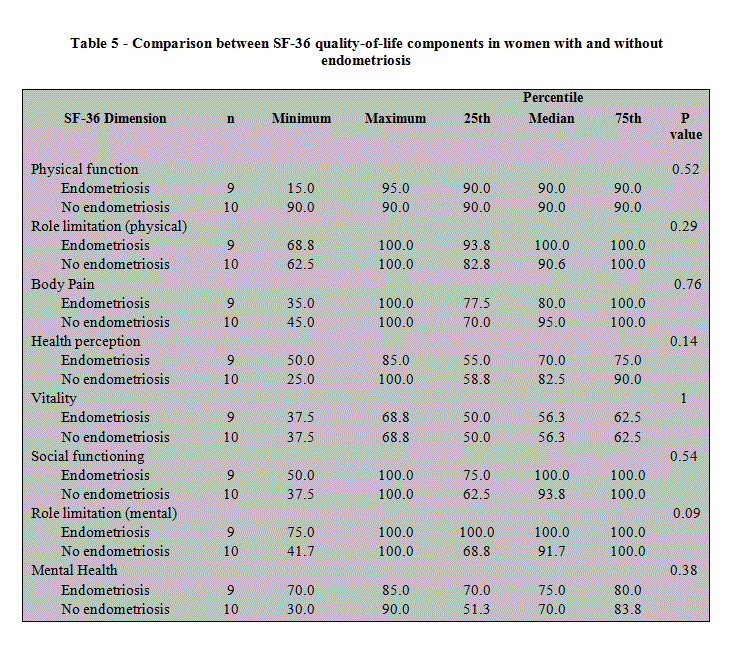
As shown in Table 4, there was generally good quality of life in the cohort of women evaluated. Compared to other dimensions of the SF-36 survey of quality of life, however, general health perception and vitality were poorer in the study population. Not surprisingly, owing to the very small sample size, there were no significant differences in dimension scores between women with endometriosis and those without (Table 5).
The recruitment figures provided a first indication of recruitment number feasibility for the main study. Following power calculations presented in the protocol, the minimum target of GSWH is to recruit at least 300 cases and 600 controls (at an estimated 30% endometriosis prevalence rate) totalling 900 women from 15 September 2008 – 31 December 2009 (28 weeks), across all 16 participating centres. Assuming similar recruitment potential across the centres, a target of 1,000 women would require recruitment of 1000/16 = 62.5 women per centre, and about one woman per week. The minimum requirement of 1,000 women over 15 months seven months is feasible.
The pilot study was successful, and showed that the target recruitment of at least 1,000 women across all centres is feasible if results from Oxford could be extrapolated to the other centres. The response rate was high, at 84.4%, and the questionnaire well received by the women. Recruitment in other centres would need to be closely monitored when the main study got underway, in order to ensure we reached the recruitment targets. Only a few textual changes were made to the content of the exposure questionnaire.